General Dentistry

Why is Preventative Care Important?
 Oral disease is entirely preventable when responsible daily oral hygiene habits at home are combined with regular professional dental care. At each appointment, our dentists and dental hygienists will provide a customized tooth cleaning accompanied by a thorough examination to detect the onset of any disease. It is our goal to help keep your smile healthy!
Oral disease is entirely preventable when responsible daily oral hygiene habits at home are combined with regular professional dental care. At each appointment, our dentists and dental hygienists will provide a customized tooth cleaning accompanied by a thorough examination to detect the onset of any disease. It is our goal to help keep your smile healthy!
While we offer a wide range of restorative dental care services for times when problems pop up, our hope is that routine dental care and preventative services will minimize your need for more extensive care.
What goes in to preventive dental care?
- Dental cleanings and hygiene: During your hygiene visits, we remove plaque from your teeth that can cause cavities and infections.
- Dental exams: A dental exam involves checking each tooth for signs of decay or damage and inspecting for possible gum disease. X-rays will possibly be taken at this appointment. If you do not bring X-rays with you, digital X-rays will be taken as needed to complete this appointment.
- Oral Cancer Screening: We examine patients for signs of mouth and/or throat cancer. The screening will consist of a visual inspection of the mouth and palpation of the jaw and neck.
- Periodontal care: Periodontal therapy is employed when you have symptoms of gum disease.
- Children’s dentistry: Children require special attention to make sure they’re developing properly and to keep cavities from forming during these vital years. That’s why our children’s dental care includes fluoride treatments and dental sealants.
 To treat a cavity, our dentist will remove the decayed portion of the tooth and then “fill” the area on the tooth where the decayed material was removed.
To treat a cavity, our dentist will remove the decayed portion of the tooth and then “fill” the area on the tooth where the decayed material was removed.
At Grove Family & Cosmetic Dentistry, we provide resin composite tooth colored fillings, which can be completed in just one visit to Grove Family & Cosmetic Dentistry. When in place, the tooth-colored filling can actually strengthen your tooth and help to prevent future decay.
Advantages of Tooth-Colored Fillings
- The tooth remains intact and stronger.
- The resin wears like natural teeth. Resin Restorations or Tooth-Colored fillings restore the natural beauty to the tooth.
The result is a beautiful smile!
Replacing Fillings with a Tooth-Colored Filling
You can have your fillings replaced with tooth-colored restorations (onlays). This process requires two appointments.
Dental Fillings or Restorations:
When a cavity is removed that area of the tooth that has been removed must be filled to protect the tooth from food impaction, cavities, and sensitivity. That material we use to fill the tooth is called a filling or restoration. Amalgam or silver filling are rarely used anymore. Today we use a composite or tooth colored material that is a resin filled with glass particles. Once the resin is placed and cured, it can be adjusted and smoothed. You’ll leave our office with a health beautiful tooth.
Resins have been available for over 20 years now and the research shows that a bonded restoration like a composite resin creates a seal with the tooth where the silver fillings did not. Resin restorations provide a wonderful replacement for natural tooth structure. Although no restoration is as strong as a natural tooth, we use resin materials that are the most advanced on the market.
Dental sealants are very thin coatings used to fill in deep grooves and pits in teeth that can harbor bacteria. They are highly effective at preventing decay on the biting surfaces of your chewing teeth.
 Sealants require a simple procedure in which a tooth-colored acrylic “coating” is painted onto the surface of the tooth. This effectively “seals” the deep grooves acting as a barrier, and protecting enamel from plaque and acids.
Sealants require a simple procedure in which a tooth-colored acrylic “coating” is painted onto the surface of the tooth. This effectively “seals” the deep grooves acting as a barrier, and protecting enamel from plaque and acids.
Benefits of Dental Sealants:
- Sealants protect the depressions and grooves of your teeth from food particles and plaque that brushing and flossing can’t reach.
- Easy to apply, sealants take only a few minutes to seal each tooth.
- Sealants hold up well under the force of normal chewing and can last several years before a reapplication is needed.
- Sealants are more affordable and less invasive to prevent cavities than it is to treat irreversible dental decay.
- Sealants are white or clear in color, making them virtually invisible when talking, smiling or eating.
- Children and adults can benefit from sealants in the fight against tooth decay
 There are times when it is necessary to remove a tooth. Some teeth are extracted because they are severely decayed; others may have advanced periodontal disease, or have broken in a way that cannot be repaired. Other teeth may need removal because they are poorly positioned in the mouth (such as impacted teeth), or in preparation for orthodontic treatment.
There are times when it is necessary to remove a tooth. Some teeth are extracted because they are severely decayed; others may have advanced periodontal disease, or have broken in a way that cannot be repaired. Other teeth may need removal because they are poorly positioned in the mouth (such as impacted teeth), or in preparation for orthodontic treatment.
The Procedure
The root of each tooth is encased within your jawbone in a “tooth socket,” and your tooth is held in that socket by a ligament. In order to extract a tooth, our dentists must expand the socket and separate the tooth from the ligament holding it in place.
At the time of extraction the doctor will need to numb your tooth, jawbone and gums that surround the area with a local anesthetic.
You feel the pressure without pain as the anesthetic has numbed the nerves stopping the transference of pain, yet the nerves that transmit pressure are not profoundly affected.
Once a tooth has been removed, neighboring teeth may shift causing problems with chewing or with your jaw joint function. To avoid these complications, we may recommend that you replace the extracted tooth.
Sectioning a tooth
Some teeth require sectioning. This is a very common procedure done when a tooth is so firmly anchored in its socket or the root is curved and the socket can’t expand enough to remove it. The doctor simply cuts the tooth into sections then removes each section one at a time.
After Care
Bleeding
Some bleeding may occur. Placing a piece of moist gauze over the empty tooth socket and biting down firmly for 45 minutes can control this. Blood clots that form in the empty socket. This is an important part of the healing process and you must be careful not to dislodge the clot.
- Avoid rinsing or spitting for 24 hours after the extraction.
- Avoid use of a straw, smoking or hot liquids.
Swelling
If swelling occurs you can place ice on your face for 10 minutes and off for 20 minutes. Repeat this cycle as you feel necessary for up to 24 hours.
Pain and Medications
If you experience pain you might use non-prescription pain relief medications such as acetaminophen or ibuprofen.
Eating
For most extractions just make sure you do your chewing away from the extraction site. Stay away from hot liquids and alcoholic beverages for 24 hours.
A liquid diet may be recommended for 24 hours.
Dry Sockets
Dry socket is when a blood clot fails to form in the socket where the tooth has been extracted or the clot has been dislodged and the healing is significantly delayed.
Following the post extraction instructions will reduce the chances of developing dry socket. Dry sockets manifest themselves as a dull throbbing pain, which doesn’t appear until three to four days after the extraction. The pain can be moderate to severe and radiate from the extraction area. Dry socket may cause a bad taste or bad breath and the extraction site appears dry.
Our doctors will apply a medicated dressing to the dry socket to sooth the pain.
Brushing and Cleaning
After the extraction avoid brushing the teeth near the extraction site for one day. After that you can resume gentle cleaning. Avoid commercial mouth rinses, as they tend to irritate the site.
Beginning 24 hours after the extraction you can rinse with salt water (1/2 teaspoon in a cup of water) after meals and before bed.
Healing
After a tooth has been extracted there will be a resulting hole in your jawbone where the tooth was. In time, this will smooth and fill in with bone. This process can take many weeks or months. However after 1- 2 weeks you should no longer notice any inconvenience.
What are inlays and onlays?
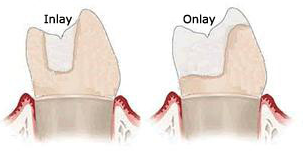 Inlays and onlays are dental restorations that are more extensive than dental fillings but less so than caps and crowns. They are typically formed in a dental lab and are made of gold, porcelain or resin depending on the patient’s needs and aesthetic goals.
Inlays and onlays are dental restorations that are more extensive than dental fillings but less so than caps and crowns. They are typically formed in a dental lab and are made of gold, porcelain or resin depending on the patient’s needs and aesthetic goals.
An inlay refers to a restoration that is formed to fit the center of a tooth, whereas an onlay refers to a restoration that encompasses at least one cusp of the tooth. Both inlays and onlays are bonded to the surface of damaged teeth and matched to the color of the surrounding teeth.
How are they applied?
Inlays and onlays require two appointments to complete the procedure. During the first visit, the filling being replaced or the damaged or decaying area of the tooth is removed, and the tooth is prepared for the inlay or onlay. To ensure proper fit and bite, an impression of the tooth taken, and sent to a lab for fabrication. Our doctors will then apply a temporary sealant on the tooth and schedule the next appointment.
At the second appointment, the temporary sealant is removed. Our doctors will then make sure that the inlay or onlay fits correctly. If the fit is satisfactory, the inlay or onlay will be bonded to the tooth with a strong resin and polished to a smooth finish.
Considerations
Traditional fillings can reduce the strength of a natural tooth by up to 50%. As an alternative, inlays and onlays, being bonded directly onto the tooth using special high-strength resins, can actually increase the strength of a tooth by up to 75%. As a result, they can last from 10 to 30 years. In some cases, where the damage to the tooth is not extensive enough to merit an entire crown, onlays can provide a very good alternative.
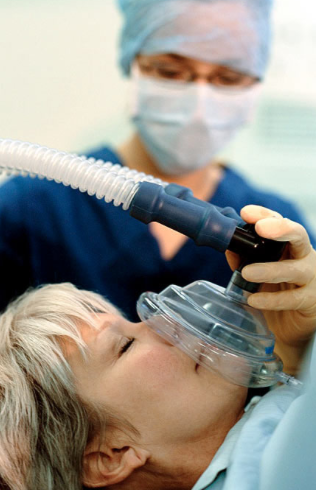 Nitrous Oxide is a sweet smelling, non-irritating, colorless gas that you can breathe.
Nitrous Oxide is a sweet smelling, non-irritating, colorless gas that you can breathe.
Nitrous Oxide (laughing gas) has been the the primary means of sedation in dentistry for many years. Nitrous oxide is safe–the patient receives 50-70% oxygen with no less than 30% nitrous oxide.
The patient is able to breathe on their own and remain in control of all bodily functions.
The patient may experience mild amnesia and may fall asleep not remembering all of what happened during their appointment.
Benefits of Using Nitrous Oxide:
- The depth of sedation can be altered at any time to increase or decrease sedation.
- There is no after effect such as a “hangover”.
- Inhalation sedation is safe with no side effects on you heart, lungs, etc.
- Inhalation sedation is very effective in minimizing gagging.
- It works rapidly as it reaches the brain within 20 seconds. In as few as 2-3 minutes its relaxation and pain-killing properties develop.
Reasons to not use Nitrous Oxide
Though there are no major contraindications to using nitrous oxide, you may not want to use it if you have emphysema, exotic chest problems, M.S., a cold or other difficulties with breathing.
You may want to ask your dentist for a “5 minute trial” to see how you feel with this type of sedation method before proceeding.
One reason people avoid or postpone needed dental treatment is, simply put, fear. While contemporary techniques allow the delivery of local anesthetic virtually pain free, memories of painful experiences from the past still haunt the dental public.  IV sedation and oral sedative techniques are an excellent alternative for treatment of such patients as well as for lengthy restorative or surgical appointments in the non phobic patient.
IV sedation and oral sedative techniques are an excellent alternative for treatment of such patients as well as for lengthy restorative or surgical appointments in the non phobic patient.
IV sedation involves the use of sedative agents administered by way of an IV line directly into the patient’s circulation. This allows the gradual dosing of appropriate medications until the patient is safely and comfortably sedated. Patients who have experienced procedures performed while undergoing IV sedation report that they feel as though they had been “put to sleep” and have no memory of any of the dental treatment. IV sedation which is extremely safe should not be confused with general anesthetic which embodies certain inherent hazards.
Oral sedation is a level of moderate sedation where a patient takes a oral medication 1 hour prior to dental treatment and that helps to relax the patient and make them less aware of the dental procedure and treatment. The dentist would still use anesthetic to get you numb prior to the procedure, but patients are much less aware of treatment taking place.
Dr. Adams is highly trained and experienced in the safe and effect use of modern IV sedation techniques.
- You may not have anything to eat or drink (including water) for six (6) hours prior to the appointment.
- No smoking at least 12 hours before surgery. Ideally, cut down or stop smoking as soon as possible prior to the day of surgery.
- A responsible adult must accompany you to the office, remain in the office during the procedure, and drive the you home.
- You should not drive a vehicle or operate any machinery for 24 hours following the anesthesia experience.
- Please wear loose fitting clothing with sleeves which can be rolled up past the elbow, and low-heeled shoes.
- Contact lenses, jewelry, and dentures must be removed at the time of surgery.
- Do not wear lipstick, excessive makeup, or nail polish on the day of surgery.
- If you have an illness such as a cold, sore throat, stomach or bowel upset, please notify the office.
- If you take routine oral medications, please check with the doctor or staff prior to your surgical date for instructions.
Your child’s first visit
 The first “regular” dental visit should be by your child’s first birthday. The first dental visit is usually short and involves very little treatment. We may ask the parent to sit in the dental chair and hold their child during the examination. The parent may also be asked to wait in the reception area during part of the visit so that a relationship can be built between your child and your dentist.
The first “regular” dental visit should be by your child’s first birthday. The first dental visit is usually short and involves very little treatment. We may ask the parent to sit in the dental chair and hold their child during the examination. The parent may also be asked to wait in the reception area during part of the visit so that a relationship can be built between your child and your dentist.
We will gently examine your child’s teeth and gums. X-rays may be taken (to reveal decay and check on the progress of your child’s permanent teeth under the gums). We may clean your child’s teeth and apply topical fluoride to help protect the teeth against decay. We will make sure your child is receiving adequate fluoride at home. Most important of all, we will review with you how to clean and care for your child’s teeth.
What should I tell my child about the first dental visit?
We are asked this question many times. We suggest you prepare your child the same way that you would before their first haircut or trip to the shoe store. Your child’s reaction to his first visit to the dentist may surprise you.
Here are some “First Visit” tips:
- Take your child for a “preview” or online tour of the office.
- Read books with them about going to the dentist.
- Review with them what the dentist will be doing at the time of the first visit.
- Speak positively about your own dental experiences.
During your child’s first visit the dentist will:
- Examine your child’s mouth, teeth and gums
- Evaluate adverse habits like thumb sucking
- Check to see if your child need Fluoride
- Teach your child about cleaning their teeth and gums
- Suggest a schedule for regular dental visits.
